Breast Reconstruction
The diagnosis of breast cancer causes a tremendous amount of fear and anxiety. After various tests, scans, MRIs, biopsies, partial mastectomies, and consultations with the surgical and medical oncologist, the patient is totally exhausted and psychologically drained. The thought of losing a breast is added to all the fears and concerns. Dr. Rafizadeh has deep empathy for this experience.
What he can tell every patient is something positive: we talk about rebuilding what is going to be taken away. This message helps the patient cope with all that lies ahead. Dr. Rafizadeh holds the patient by the hand and goes through this journey with them. They require a lot of tender love and care — and he is the last person they see when all the treatments are done. That is when he puts the final touch on their reconstructive process.
“I really feel all these anxieties and fears when I first see the patients in my office. Luckily what I have to tell a patient is something positive. We talk about rebuilding what is going to be taken away. This message helps the patient cope with all that lies ahead. I hold the patient by the hand and go through this journey with them.”
— Dr. Farhad Rafizadeh, MD FACS
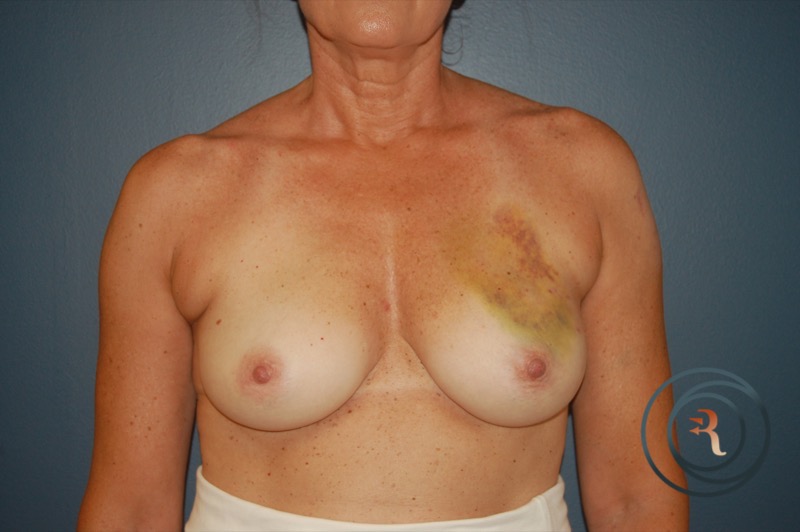
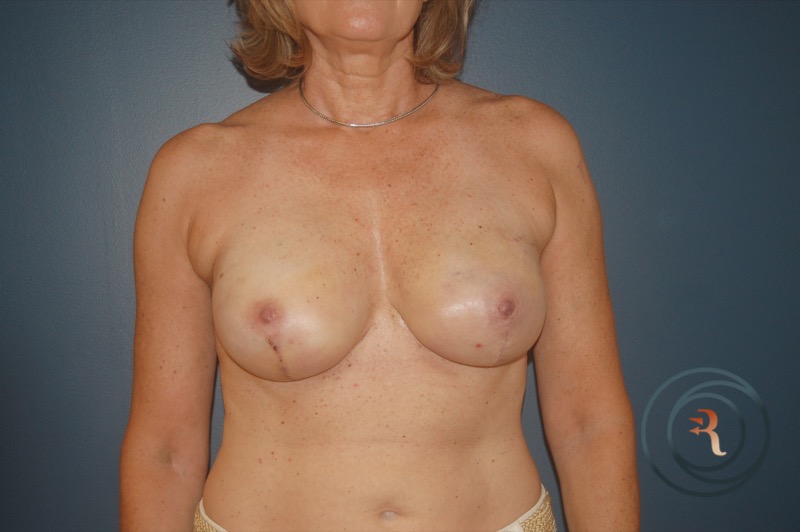
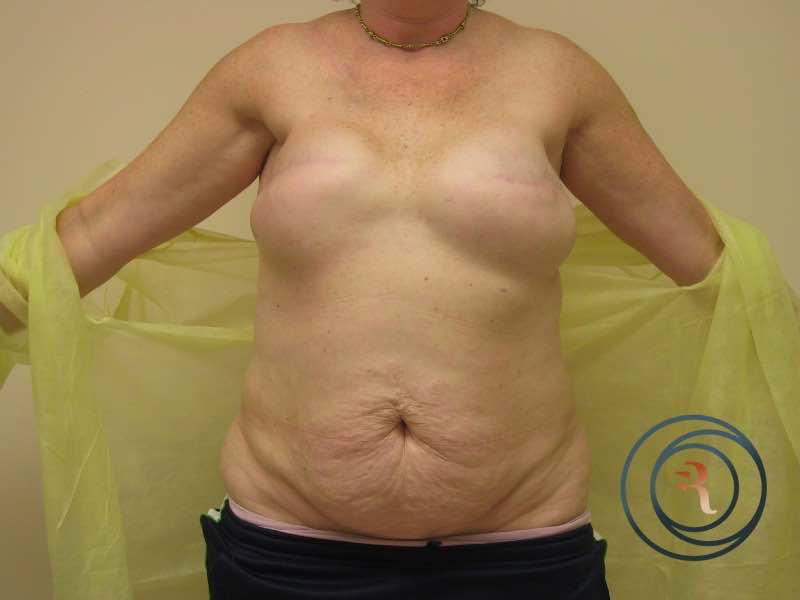
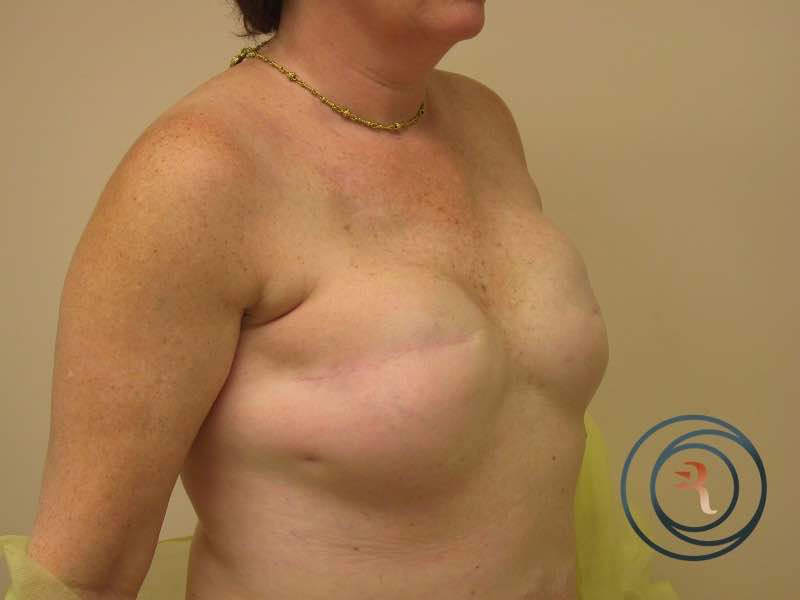
Implant-Based Reconstruction
Implant-based reconstruction is the most common approach. It may be performed in one or two stages. In immediate one-stage reconstruction, an implant is placed at the time of mastectomy. In a two-stage approach, a tissue expander is placed at mastectomy and gradually filled over weeks to stretch the skin envelope; the expander is then exchanged for a permanent implant in a second procedure. The choice depends on whether the patient is having radiation therapy, the quality of the mastectomy skin flaps, and patient preference.
Tissue-Based Reconstruction
Tissue-based reconstruction uses the patient's own tissue from another area of the body to reconstruct the breast mound. The most common donor sites are the abdomen (TRAM flap or DIEP flap) and the back (latissimus dorsi flap). Tissue-based reconstruction produces a more natural result and is particularly advantageous for patients who have had or will have radiation therapy. Dr. Rafizadeh has performed breast reconstruction with patients' own tissues for many years, which has also refined his mastery of all breast procedures.
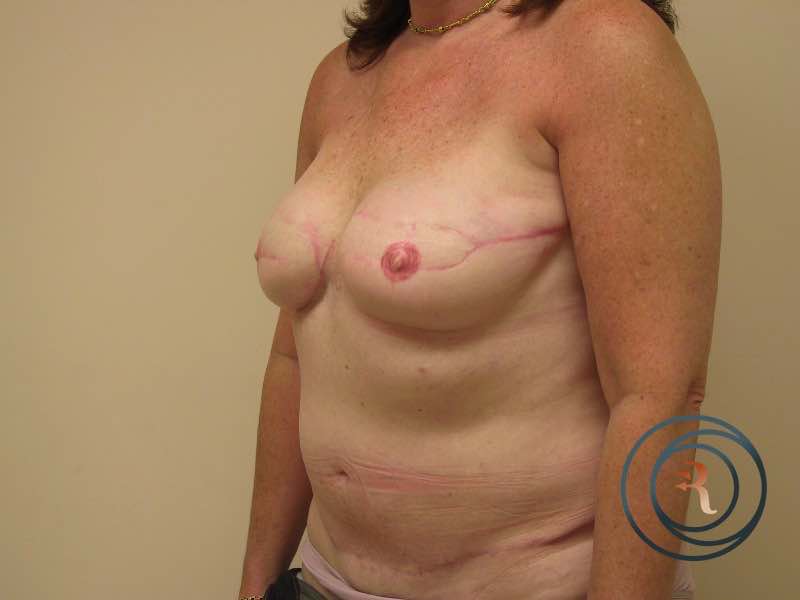
Nipple & Areola Reconstruction
The final stage of breast reconstruction — nipple and areola reconstruction — is typically performed several months after the primary reconstruction, once the breast mound has settled. The nipple projection is created using local flap techniques, and the areola color is restored using medical-grade tattooing. This final step completes the reconstruction and is an important part of the patient's psychological recovery.
Insurance Coverage
Under the Women's Health and Cancer Rights Act of 1998 (WHCRA), insurance plans that cover mastectomy are required to also cover breast reconstruction. This includes reconstruction of both breasts to achieve symmetry. Dr. Rafizadeh's office works closely with patients to navigate the insurance authorization process.